
Whoopee! Next month it’s my 67th birthday and this blog, #VixView, is my celebration of life. The goal is to stay alive for three more years. Why three years, I hear you ask?
Dying early -the magic of 70
Let’s blame it on the United Nations and the Sustainable Development Goal number 3 target 3.4:
By 2030 reduce by one-third pre-mature mortality from non-communicable diseases (NCDs) through prevention and treatment, and promote mental health and wellbeing
So if I die between the ages of 30 and 70 years, it is too soon. Well not me specifically, but people who live with non-communicable diseases (NCDs). You get the drift – so I am hanging in for 3 more years. It sounds a bit like an electioneering slogan. But it isn’t. It’s deadly serious. Really.
An activist – why me?
Today I coexist with over 20 health conditions, all NCDs, with the first illness, psoriasis, starting in my first 500 days. I have a most productive and interesting life despite this seemingly woeful state of my health.
Being an NCDs activist gripped me tighter each time I survived another near-death experience (NDEs). Trust me, NDEs change one’s perspective, one’s way of being. I found that to live, I had to fight for my life. So that’s what I do and along the way, I do it for and with those who living with NCDs. I learned radical self-care.
Note: Don’t scoff too much about NDEs. Remember Angelo Agrizzi and what he did after his NDE?
50 years on
 If that isn’t enough, this is my 50th year as a health professional working in the health sector. It feels like an alien place. I have a 360º view through all the learning and experience. My beacon remains the Alma Ata vision of primary health care.
If that isn’t enough, this is my 50th year as a health professional working in the health sector. It feels like an alien place. I have a 360º view through all the learning and experience. My beacon remains the Alma Ata vision of primary health care.
Today, with profound sadness, I see us facing many of the challenges from when I first began back in 1970. I recognise that the health system in our noble land often fails us, its people, irrespective of where we get care: public or private. Evidence is all around.
Travel with me
So join me and find out if I make it. #VixView
Click here to download the SA Health Promotion Policy & Strategy 2015-19 (HPP&S 15-19)
46 pages. Date of publication: unknown
Purposes
1.To enable South African to increase control over and improve its own health using the PHC approach, which is multidisciplinary in nature;
2.To provide guidelines to support actions at appropriate levels that will advance the aims and objectives of the health promotion policy;
3.To promote a holistic approach to health by:
- Focus on the link between health promotion and the determinants of health
- Emphasise inter-sectoral and multi-disciplinary approaches in planning, implementing and evaluating health promotion interventions;
- Outline health promotion activities in various settings; and
- Specifying strategic indicators to be monitored
Target audiences
The HPP&S 15-19 identifies key target audiences across the life cycle for health promotion interventions (→ focus on)
- Children < 5 years → promoting better health;
- Women of child bearing age → creating awareness on services available;
- Men → promoting a change in gender norms and values by encouraging broader involvement in health issues;
- Youth → addressing risky behaviour and promoting healthy lifestyle practices;
- Older people → community-based programmes and support groups to promote regular health and self-management of NCDs;
- Marginalised populations → specific health needs.
Snippets
12.2 Financial Resources (page 26)
The successful implementation of the health promotion programme requires sustained and dedicated financial resources. The allocation of resources should be based on the principles of redress and equity. The current financial resources limits the implementation of health promotion strategies that are known to increase awareness on critical health issues and impact upon on social and behavioural changes that promote health and well being.
Civil society role – key partners (page 29-30)
- Developing and promoting frameworks for health promotion interventions
- Strengthening partnerships with community structures and civil society for health campaigns
- Supporting PHC Ward-Based Outreach Teams to implement health promotion programmes with activities to develop:
-a package of service delivery of health promotion services
-tools to assess and promote community mobilisation.
- Improving health literacy.
Chronic Care Model/ Self-management /Patient centred care
Where is South African in its response to person-centred NCDs care?
The national Department of Health is putting its money and credibility behind its Integrated Chronic Disease Management (ICDM) Model with little consultation. (Integrated Chronic Disease Management: A step by step manual to guide implementation. Undated. Authors Dr Shaidah Asmall and Dr Ozayr Mahomed). This ICDM model is also cited as being integral to the NCD Strategic Plan.
Mahomed). This ICDM model is also cited as being integral to the NCD Strategic Plan.
The SA NCD Alliance is putting forward two key aspects that are import for patients, people living with NCDs. These are
• PATIENT –CENTRED CARE AKA PERSON-CENTRED CARE
• SELF-MANAGEMENT (not assisted)
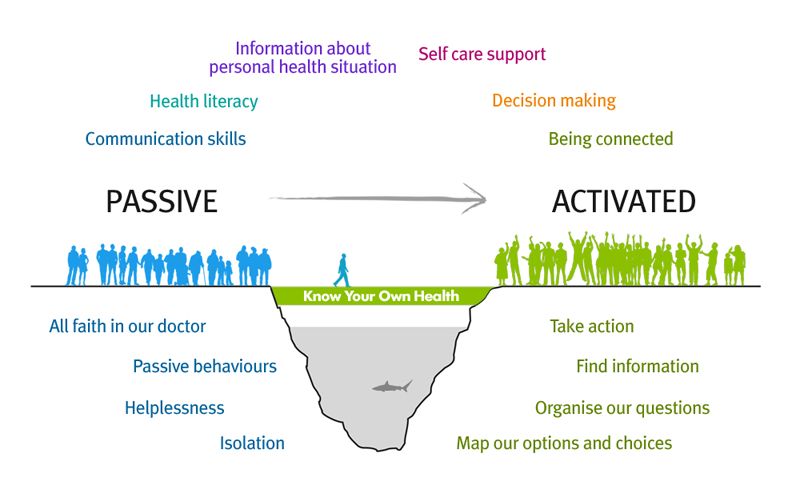
What is person-centred care?
A person-centred health system is one that supports people to make informed decisions about, and to successfully manage, their own health and care, able to make informed decisions and choose when to invite others to act on their behalf. This requires healthcare services to work in partnership to deliver care responsive to people’s individual abilities, preferences, lifestyles and goals.
The goal of person-centred care is to allow the patient to successfully manage their own health care – self-management. Self-management is one of the pillars for high quality care in the US Institute of Medicine’s definition.
Self management support is the job of the health care system it is fundamental and not an added extra. It is provided through graded active support.
There has be little or no consultation by the Department of Health with patients or patient group or caregivers about these matters. So we are putting up two references that back their importance.
“Self management supportcan be viewed in two ways: as a portfolio of techniques and tools that help patients choose healthy behaviours; and a fundamental transformation of the patient-caregiver relationship into a collaborative partnership.”
Bodenheimer T, MacGregor K, Shafiri C (2005). Helping Patients Manage Their Chronic Conditions. California: California Healthcare Foundation
Further information on self management support can be found at www.health.org.uk/sms
The 2 resources listed below are very informative:
The Theory and evidence behind self management. Slide presentation by Natalie Grazin, Assistant Director of The Health Foundation
A particularly important slide set that integrated the chronic care from the perspective of the patient – person living with an NCD. It highlights how much change is necessary to implement such a model in current most chronic care settings.
Helping measure person-centred care A review of evidence about commonly used approaches and tools used to help measure person-centred care 2014 The Health Foundation: London by Dr Debra de Silva
This is an easy to ready snapshot of person-centred care with showing tools that can be used to measure different aspects of self-management.

 If that isn’t enough, this is my 50th year as a health professional working in the health sector. It feels like an alien place. I have a 360º view through all the learning and experience. My beacon remains the Alma Ata vision of primary health care.
If that isn’t enough, this is my 50th year as a health professional working in the health sector. It feels like an alien place. I have a 360º view through all the learning and experience. My beacon remains the Alma Ata vision of primary health care.


 Mahomed
Mahomed