
Geneva, 14 March 2024– A major new study released by The Lancet Neurology shows that, in 2021, more than 3 billion people worldwide were living with a neurological condition. The World Health Organization (WHO) contributed to the analysis of the Global Burden of Disease, Injuries, and Risk Factor Study (GBD) 2021 data.
Neurological conditions are now the leading cause of ill health and disability worldwide. The overall amount of disability, illness and premature death (known as disability-adjusted life years, DALYs) caused by neurological conditions has increased by 18% since 1990.
Over 80% of neurological deaths and health loss occur in low- and middle-income countries, and access to treatment varies widely: high-income countries have up to 70 times more neurological professionals per 100 000 people than low- and middle-income countries.
“Neurological conditions cause great suffering to the individuals and families they affect, and rob communities and economies of human capital,” said Dr Tedros Adhanom Ghebreyesus, WHO Director-General. “This study should serve as an urgent call to action to scale up targeted interventions to allow the growing number of people living with neurological conditions to access the quality care, treatment and rehabilitation they need. It is more important than ever to ensure brain health is better understood, valued and protected, from early childhood to later life.”
The top ten neurological conditions contributing to loss of health in 2021 were stroke, neonatal encephalopathy (brain injury), migraine, dementia, diabetic neuropathy (nerve damage), meningitis, epilepsy, neurological complications from preterm birth, autism spectrum disorder, and nervous system cancers.
Overall, neurological conditions cause more disability and health loss in men compared to women, but there are some conditions like migraine or dementia where women are disproportionately affected.
Since 1990, the absolute number of individuals living with, or dying from, neurological conditions has increased, while age-standardized DALY rates have dropped. This means that increases in absolute numbers are mainly driven by demographic change and people living longer.
Diabetic neuropathy was the fastest growing neurological condition. The number of people with diabetic neuropathy has more than tripled globally since 1990, rising to 206 million cases in 2021. This increase is in line with the worldwide increase in diabetes. Other conditions such as neurological complications from COVID-19 (for example, cognitive impairment and Guillain-Barré syndrome) did previously not exist and now account for over 23 million cases.
At the same time, neurological burden and health loss due to other conditions decreased by 25% or more since 1990 as a result of improved prevention (including vaccines), care and research: tetanus, rabies, meningitis, neural tube defects, stroke, neurocysticercosis (parasitic infection that affects the central nervous system), encephalitis (inflammation of the brain), and neonatal encephalopathy (brain injury).
The study also examined 20 modifiable risk factors for potentially preventable neurological conditions such as stroke, dementia and idiopathic intellectual disability.
Eliminating key risk factors – most importantly, high systolic blood pressure and ambient and household air pollution – could prevent up to 84% of stroke DALYs. Similarly, preventing exposure to lead could reduce the burden of idiopathic intellectual disability by 63.1%, and reducing high fasting plasma glucose levels could reduce the burden of dementia by 14.6%. Smoking significantly contributed to stroke, dementia and multiple sclerosis risk.
More investments needed to improve treatment, care and quality of life
At the World Health Assembly in 2022, Member States adopted the Intersectoral global action plan on epilepsy and other neurological disorders 2022–2031 (IGAP) with ambitious scope to address the long standing neglect of neurological disorders.
“The Intersectoral Global Action Plan 2022–2031 sets out a roadmap for countries to improve prevention, early identification, treatment and rehabilitation of neurological disorders. To achieve equity and access to quality care, we also need to invest in more research on risks to brain health, improved support for the healthcare workforce and adequate services,” said Dévora Kestel, Director, WHO Department of Mental Health and Substance Use.
IGAP sets out strategic objectives and targets to improve access to treatment, care and support for people with neurological disorders; implement strategies for brain health promotion and disease prevention; strengthen research and data; and emphasize a public health approach to epilepsy and other neurological disorders.

Non-communicable diseases (NCDs) appear to be rising in priority for the first time in more than two decades since the publication of the South African National Development Plan (NDP). The recent NDP 10-year review seems to frame NCDs in a different light by making this recommendation:O
Department of Health should implement the legislative and regulatory interventions recommended by the Strategic Plan for the Prevention and Control of Non-Communicable Diseases.” page 39

The recommendation appears to open the way for a national policy shift, moving NCDs out of the rut that considers them solely lifestyle conditions managed by a mixture of behaviour changes with a mix of policy and fiscal measures. This NDP framing institutionalised the limited allocation of national budget resources for NCDs interventions officially sanctioned as primordial and primary prevention. In reality, it resulted in NCD denialism despite them being the leading cause of death in South Africa since 2009, once ARVs impacted the tragic and callous loss of life due to HIV.
The use of the term lifestyle conditions is unacceptable for the HIV and TB community. People living with NCDs+ find it equally demeaning as it places the responsibility mainly on the person to live a better life.This bogus notion disregards the wider or social determinants of health and a public health system that fails to prevent and treat NCDs in a comprehensive way in all primary care facilities.
Very little changed for 20 years with subsequent NDP iterations of health priorties which continue to feature the Millennium Development Agenda identified conditions and South Africa’s much delayed and controversial version of universal health coverage. National Health Insurance (NHI) draft legislation focuses only finacial mechanism and fails to deal with quality and equity for NCDs and mental health.
Be still my heart NCDs equity indicator
Being a cynic in NCDs matters, when I look at policies I look first at the list of acronyms which usually feature up front. Very quickly I notice that the acronym NCDs does not appear in this standard feature South African policy documents. In most health-related policies, NCDs, the acronym, is missing with little or no mention within the policy and, unsurprisingly, even less action.
I made my first indicator of NCDs policy equity to be the inclusion of NCDs in the list of acronyms. Why? It give a snapshot of the framing from the perspective of the policymakers. So it is a huge milestone to have NCDs finally made the acronym indicator cut. NCDs has appear in this review and, be still my heart, in the recently update HIV/TB & STIs national strategic plan. Using the criterion in reverse, it is intriguing that neither HIV nor AIDS makes this list, but TB does. Perhaps is shows the extent to which HIV is institutionalised in South African society.
In a related victory, NCDs featured for the first time in the acronym list of the HIV, TB and STIs stratgic plan!
Hope springs eternal
It took the South African NCDs+ Alliance 10 years and lots of activism to be included in the development of the NCDs+ National Strategic Plan. Real blood, sweat and tears stuff. We had to take extreme measures including delaying tactics and staking sham policy consultations. After 5 years of delays it was finally passed and launched last year. It does allow scope for increasing the priority of NCDs prevention and treatment. However, without futher clarification of the NDP review recommendation is nuanced. What do “legislative and regulatory interventions” mean? Is it just another way of maintaining the status quo?
Make this cynic think paranoid thoughts. Especially as the health minister and officials havent responded to letters for years. What do you think?
The SANCDA’s founding partners ask the Minister of Health, Dr Joe Phaahla, to work together to solve the NCD epidemic sent 19 April 2023. Still awaiting a response. From 2013 until today, the SANCDA has never received a written response from its political leadership or executive officials.
Summary of contents
- Annexure A: SANCDA members, allies, and partners.
- Annexure B: List of policy requiring coordination and update by date and government Department
- Annexure C: Contextualisaton of NDOH NCDS+ subprogramme allocations (1010-2026) with the Health Promotion Leavy and & HIV NPOs
SANCDA Letter to Minister Apr 2023 and annexures A B C
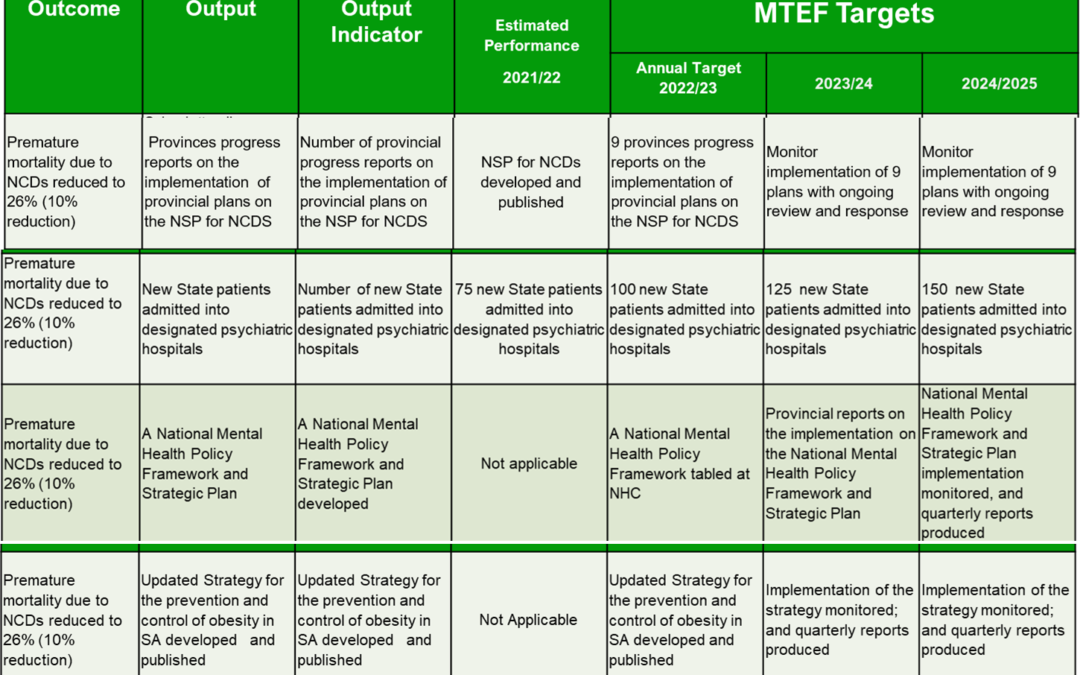
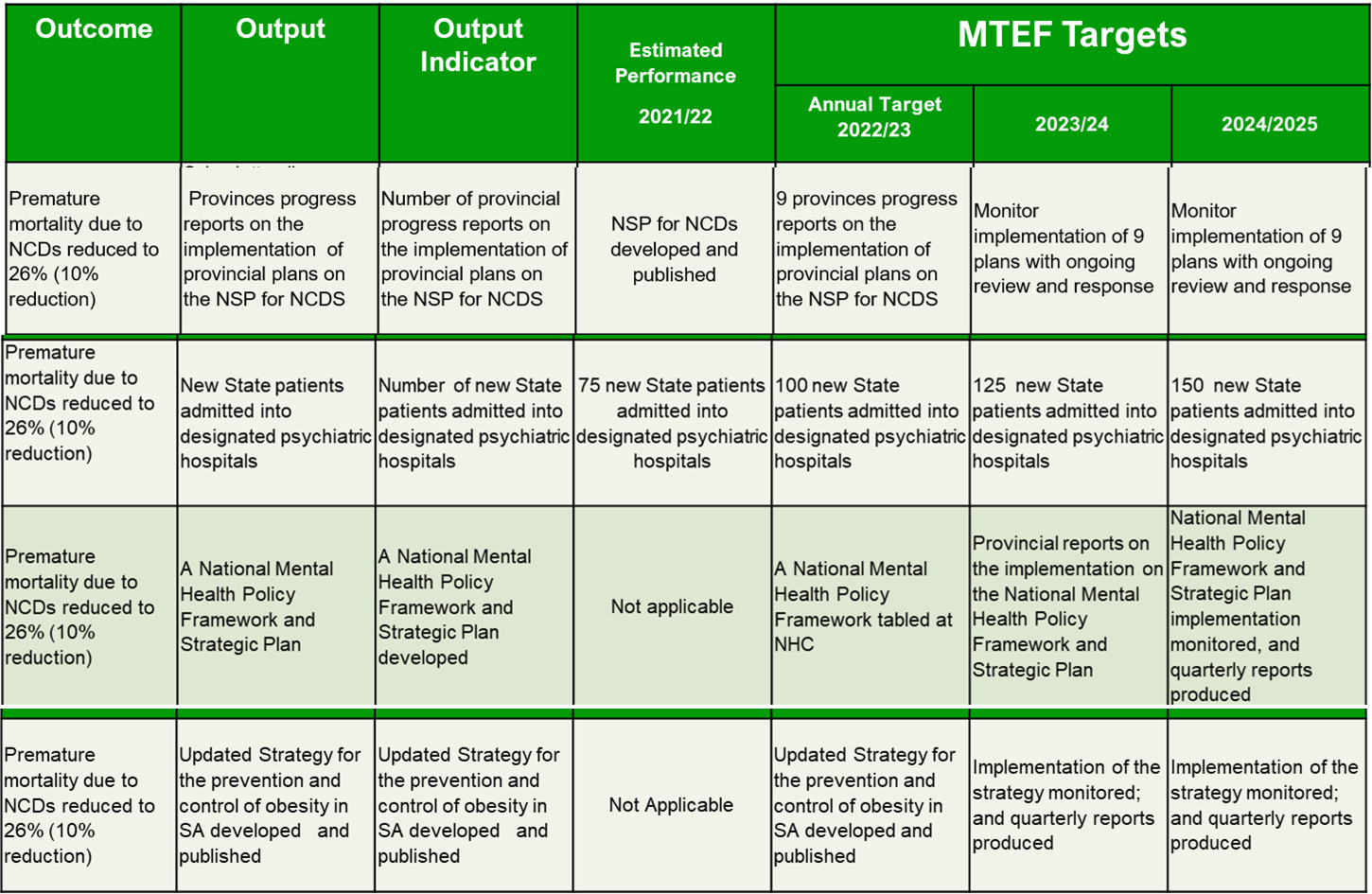
NCDs related outcomes for APP 202s/2023
NCDs are a neglected priority in the National Department of Health (NDoH) Annual Performance Plan 2022/23 (APP) which expires at the end of March. Only 4 /18 outcomes in programme 3 are NCD-related.
The bottom 2 rows in the table, require the re-development of national policies for mental health and obesity. Transparency and an inclusive process are problematic.
Our Constitution calls for the meaningfu involvement of civil society and people living with NCDs. Together these conditions impact millions of South Africans and place increasing burden on the health system.
It would also be great to see the reviews of the existing policies which should come before a new policy.
The NCDs+ National Strategic Plan 2022-2027, launched in May 2023, (see the top row in the table) Implying that the provinces will have be close to publishing the impemetion plans for obesity, diabetes and hypertension. I know there is lots hard work getting the plans ready. The Medium-Term Strategic Framework 2019-24 makes it clear that NCDs budgets and implementation must happend in at the sumbnational or provinical level.






